The Hidden Cost of Payer Portals on your Practice Overhead
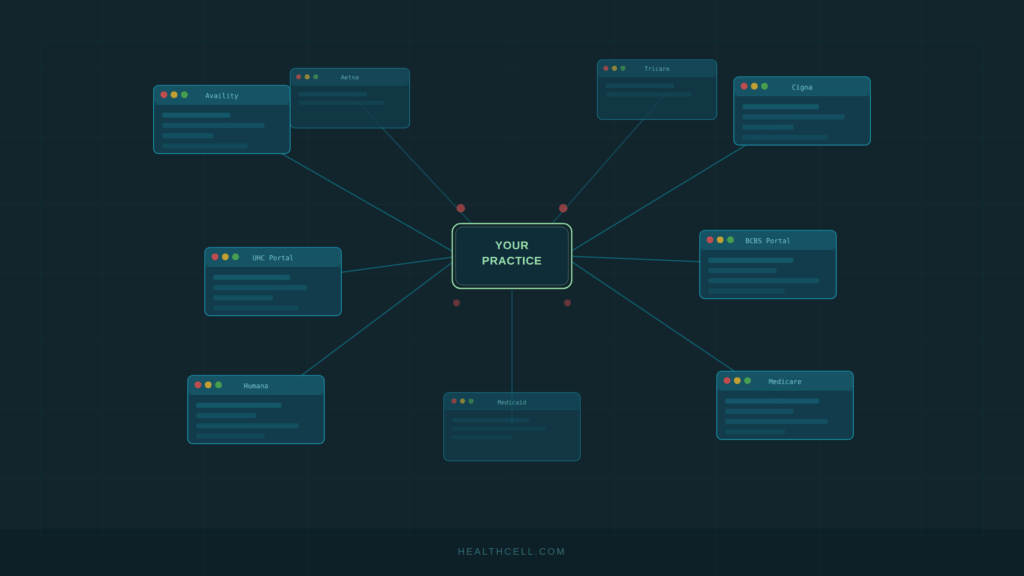
Payer portals are one of those operational realities that every medical practice lives with but rarely talks about as a standalone problem. Your billing team logs into Availity, then UnitedHealthcare, then Humana, then Aetna — re-entering patient data at every stop — and by mid-morning, they’ve touched half a dozen disconnected systems just to do […]
What the 2027 CMS Advance Notice Means for Independent Practices

The Centers for Medicare & Medicaid Services (CMS) recently released its 2027 Medicare Advantage (MA) and Part D Advance Notice, offering an early look at how the agency plans to set payment rates and risk adjustment policies in the coming years. While the notice is directed at Medicare Advantage plans, its implications extend well beyond […]
When Should a Small Practice Consider Outsourcing Their Prior-Authorization Process?

Prior Authorization as a Silent Profit Erosion Engine Prior authorization is no longer a background administrative task. It has evolved into a high-friction, high-cost operational function that quietly erodes profitability, clinical efficiency, and staff morale. For small practices, the danger lies not in the existence of prior authorization itself, but in tolerating its expanding footprint […]
When In-House Billing Becomes More Expensive Than Outsourcing

If your billing team feels constantly overwhelmed—but your collections aren’t improving—you’re not alone. Many medical practices reach a point where in-house billing quietly becomes more expensive than they realize. Early on, managing billing internally often makes sense. It offers control, familiarity, and the perception of lower costs. But as practices grow and reimbursement becomes more […]
Dermatology Billing and Coding in 2026: What Practices Need to Prepare For

Dermatology practices in 2026 won’t see a dramatic across-the-board crash in reimbursement—but there will be real pressure in specific places. The biggest disruptor is the overhaul of skin substitute reimbursement, layered on top of ongoing tightening around documentation, coding accuracy, and MIPS performance. Practices that simply “roll over” their 2025 workflows into 2026 risk margin […]
Coding Changes Impacting Cardiology Practices in 2026

The 2026 coding year represents one of the most significant regulatory shifts cardiology practices have faced in more than a decade. Unlike routine annual updates, the changes taking effect Jan. 1, 2026, combine large-scale CPT restructuring, expanded ICD-10 specificity, and meaningful Medicare reimbursement policy adjustments that directly affect interventional, imaging, electrophysiology, and chronic care services. […]
10 Practical Ways to Transform the Patient Waiting Room Experience

For all the advancements in digital health, smart scheduling, and virtual care, the patient waiting room remains one of the most influential touchpoints in a patient’s journey. It’s often the first in-person impression patients have of a practice, and it can shape how they perceive the quality of care long before they meet a clinician. […]
What you Need to Know About the CMS’s WISeR Model and Impact on Prior-Authorization Requirements

For years, prior authorization has been a defining feature of Medicare Advantage and commercial health plans. Traditional Medicare, however, has largely avoided it — until now. Beginning Jan. 1, 2026, the Centers for Medicare & Medicaid Services (CMS) will launch one of its most significant oversight experiments yet: the Wasteful and Inappropriate Services Reduction (WISeR) […]
A Practical Guide to Creating an Effective Medical Office No-Show Policy

Missed appointments may seem like a small inconvenience, but they add up fast. Studies show that medical practices lose an estimated $150–$200 for every no-show, and with no-show rates commonly ranging from 10 to 30 percent, the impact on access, staffing, and revenue becomes impossible to ignore. When a patient doesn’t arrive for a scheduled […]
Top Independent Physician Associations to Consider in 2026

Independent practices are navigating a complicated moment in health care. Administrative burdens continue to rise, payer contracting grows more complex each year, and value-based care models increasingly require data and reporting infrastructure that is often out of reach for solo or small groups. Against that backdrop, Independent Physician Associations (IPAs) have re-emerged as one of […]