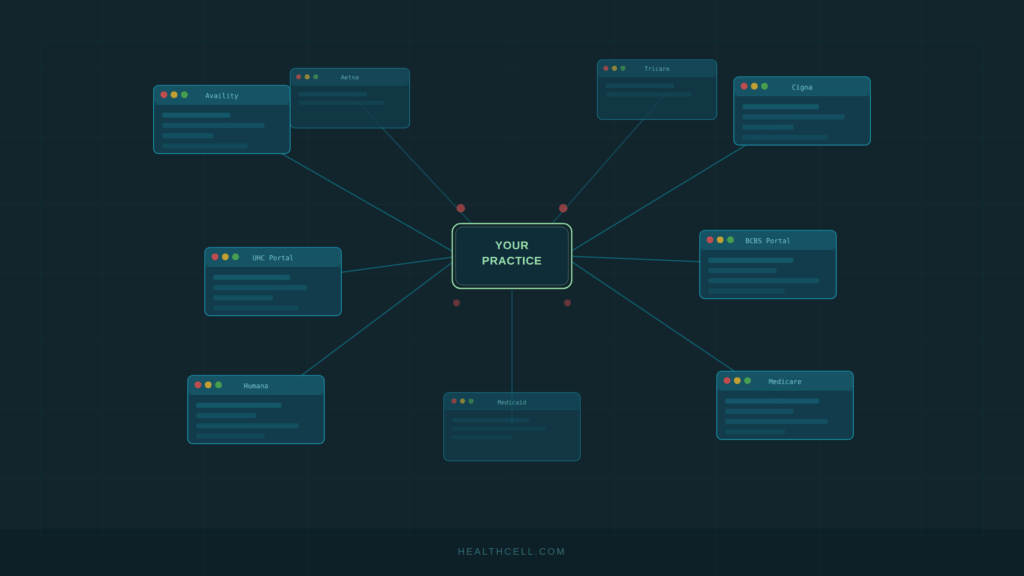
Payer portals are one of those operational realities that every medical practice lives with but rarely talks about as a standalone problem. Your billing team logs into Availity, then UnitedHealthcare, then Humana, then Aetna — re-entering patient data at every stop — and by mid-morning, they’ve touched half a dozen disconnected systems just to do work that a single query should have handled.
A recent MGMA Stat poll published April 1, 2026, puts hard numbers behind the frustration: 61% of medical practices report their staff access seven or more payer portals every single week. More than a quarter are logging into 11 or more. Only 10% of practices manage to keep it to three or fewer.
For practice leaders already stretched thin on staffing and revenue cycle performance, those numbers deserve a closer look.
How Payer Portals Create Hidden Operational Overhead
The portals themselves aren’t broken — they exist and they mostly function. The problem is that each payer portal operates as its own universe. Different logins. Different navigation. Different search behaviors. Different timeout rules. Different terminology for the same claim statuses. Staff who handle payer interactions end up building payer-specific muscle memory — not because the work itself varies, but because the interfaces demand it.
A single prior authorization can require a staff member to confirm eligibility in one payer portal, submit the auth request in another, check status in a third, and document the outcome back in the EHR — which connects natively to none of them. Multiply that by dozens of cases per day, and the arithmetic gets heavy fast.
According to MGMA respondents, the most frequently cited pain points weren’t about any single payer portal being poorly designed. They were about the cumulative burden: maintaining multiple credentials, dealing with frequent timeouts and re-authentication, navigating inconsistent interfaces, and being forced out of the EHR into manual workflows across portals that should have been unnecessary.
The Real Cost of Managing Too Many Payer Portals
Payer portal sprawl is ultimately a staffing and resource allocation problem. Every hour a billing or authorization specialist spends navigating disconnected portals is an hour not spent on follow-up, denial resolution, patient communication, or process improvement.
The MGMA article frames it well: the question isn’t whether payer portals are frustrating — everyone already knows that. The question is whether the portal workload is visible enough in your staffing models and productivity expectations to be managed deliberately, or whether it’s buried inside broader task categories where the true cost never gets measured.
For most practices, it’s buried. And that invisibility is expensive. When practices report they can’t keep up with prior authorization volume or that denials are taking too long to work, part of the diagnosis should include how much staff capacity is being consumed by the mechanical overhead of payer portal access alone.
Why Payer Portal Fragmentation Isn’t Going Away
Payers have no incentive to standardize their portals, and corporate-level consolidation among insurance companies hasn’t translated into portal consolidation at the practice level. Acquisitions often mean more payer portals, not fewer, as legacy systems from absorbed companies persist under the same parent organization.
Clearinghouse tools and middleware can help with certain tasks like eligibility checks and claims status lookups, but prior authorization submissions, appeal workflows, and plan-specific documentation requirements still frequently route staff right back to individual payer portals. The consolidation is rarely complete.
The 2024 Change Healthcare outage made things worse for many practices that were forced to rebuild manual payer portal workflows under pressure — and some never fully migrated back. For smaller or resource-constrained groups, the manual workarounds became the new default simply because there was no capacity to manage another transition.
Regulatory changes like the CMS Interoperability and Prior Authorization Final Rule, which requires standardized FHIR API data exchange from payers by January 2027, hold promise for reducing reliance on individual payer portals over time. But that’s a timeline measured in years, not weeks. Your practice needs relief now.
How to Get Payer Portals Off Your Team’s Plate
This is exactly the kind of operational burden that a dedicated revenue cycle partner is built to absorb. Rather than training your staff to maintain fluency across a growing number of payer portals, you can offload the two tasks that drive the majority of portal use — eligibility verification and prior authorization — to a team that manages them full-time.
At HealthCell, our Pre-Visit Assurance service handles eligibility verification and prior authorization before the patient ever walks through your door. We manage the payer portal logins, the payer-specific requirements, the follow-ups, and the re-submissions so your staff doesn’t have to.
And unlike a clearinghouse that handles only part of the workflow, Pre-Visit Assurance is available as a standalone service. You don’t have to overhaul your entire billing operation to get the payer portal burden off your team. Whether you need full end-to-end RCM or targeted help with eligibility and authorizations, HealthCell can meet you where you are.
What that looks like in practice:
Eligibility verified before every visit — no more front-desk surprises or post-visit claim rejections because coverage lapsed or benefits weren’t confirmed.
Prior authorizations submitted and tracked across payer portals — managed by specialists who maintain the payer-specific fluency your team shouldn’t have to build.
Your staff stays in the EHR — instead of context-switching between six, eight, or 11 different payer portals every morning.
Fewer denials on the back end — because the verification and authorization work was done right the first time, in the right portal, with the right documentation.
Stop Absorbing a Payer Portal Problem That Isn’t Yours to Solve
Payer portal fragmentation is an industry-level failure that individual practices are forced to absorb at the operational level. You can’t fix it. You can’t standardize it. You can’t wait for regulation to fix it. But you can stop letting it consume your team’s time and attention.
If your staff is spending their mornings logging in and out of payer portals instead of working claims, resolving denials, or improving patient communication, it’s time to talk about a different model. Learn more about HealthCell’s Pre-Visit Assurance service and find out how we can take the payer portal burden off your plate — starting in as little as two weeks.