Why Provider Credentialing Continues to Disrupt Practices
In 2026, provider credentialing and payer enrollment still rank among the most persistent causes of delayed cash flow, avoidable denials, and elevated compliance exposure for small and mid-sized medical practices. Minor oversights can have outsized consequences. A single lapse may sideline a new provider’s clinic schedule for months, turn otherwise clean claims into rejections, or leave the organization vulnerable to audits and payer clawbacks.
This guide breaks credentialing down in straightforward terms. It presents a pragmatic, real-world workflow designed for independent practices and calls out the moments when outside expertise—such as support from a seasoned revenue cycle partner like HealthCell—can reduce friction, protect revenue, and restore operational momentum.

Credentialing, Enrollment, and CAQH: Defining the Landscape
Before any workflow takes shape, practices must agree on the language. Terminology gaps may seem benign, but they are often the root cause of internal confusion, stalled applications, and fractured accountability.
| Term | Purpose | Key Outcome |
|---|---|---|
| Provider Credentialing | Verifies qualifications & background | Compliance approval |
| Payer Enrollment | Registers provider with insurance plans | Ability to bill & get paid |
| CAQH ProView | Centralized credentialing data repository | Faster commercial enrollment |
Provider credentialing
Provider credentialing is the formal validation of a clinician’s professional background. It encompasses education, postgraduate training, active licenses, board certifications, employment history, malpractice coverage, and any record of sanctions or disciplinary actions. A central component is primary source verification (PSV), in which the practice, a payer, or a credentials verification organization (CVO) confirms credentials directly with issuing institutions—medical schools, residency programs, state licensing boards, and certifying authorities.
At its core, credentialing answers a simple but critical question: Is this clinician who they claim to be, and are they appropriately qualified to provide care?
Payer enrollment (provider enrollment)
Payer enrollment runs parallel to provider credentialing but serves a different purpose. It is the process of registering a provider with specific insurance plans—Medicare, Medicaid, commercial carriers, Medicare Advantage—so the provider is recognized as in-network and eligible for reimbursement. The work includes submitting payer-specific applications or electronic forms, executing participation agreements, and securing provider IDs and effective dates.
Enrollment answers a more transactional question: Can this provider be paid by this plan, within this practice, starting on a defined date?
CAQH and centralized provider data
The Council for Affordable Quality Healthcare (CAQH) manages CAQH ProView, a centralized database where providers maintain credentialing profiles accessed by many commercial payers. Providers are required to attest to the accuracy of their information at least every 120 days—180 days in Illinois. Miss that window, and the profile can lapse into an expired status, interrupting payer visibility and slowing credentialing activity.
Today, a complete and meticulously maintained CAQH profile is no longer a differentiator. It is baseline infrastructure for efficient commercial credentialing and recredentialing.
How Provider Credentialing Shapes Revenue and Compliance
Credentialing is often mislabeled as administrative overhead. In reality, it is a frontline revenue safeguard and a foundational compliance control.
Revenue impact
When providers begin treating insured patients before credentialing and enrollment are complete, claim denials are almost inevitable. “Out of network.” “Provider not on file.” The language varies, but the result is the same—no payment.
Many payers refuse to retroactively enroll providers to their first day in clinic. The consequence is blunt. Practices are left to absorb the loss, write off visits, or reclassify encounters as discounted self-pay.
Industry analyses consistently point to incomplete or inaccurate applications as a primary driver of enrollment delays and outright rejections. The downstream effect is slower onboarding, disrupted scheduling, and constricted cash flow.
Put plainly, every week a full-time provider sits in credentialing limbo can cost a practice thousands of dollars in deferred or unrecoverable revenue.
Compliance and audit exposure
Credentialing failures carry regulatory consequences as well. Accrediting organizations, state licensing boards, and CMS expect credentialing files to be comprehensive and current, and they routinely examine them during audits and surveys.
Thin or disorganized documentation increases malpractice exposure and weakens a practice’s position if a quality-of-care or patient safety event occurs.
Medicare raises the stakes further. Inaccurate or outdated PECOS records—such as unreported ownership changes, practice locations, or adverse actions—can trigger billing privilege revocations and retroactive payment recoupments.
For independent practices, credentialing is therefore not a side task. It is an integral component of revenue cycle integrity and corporate compliance discipline.
The End-to-End Provider Credentialing Workflow
Effective credentialing does not happen by accident. It relies on a documented, repeatable workflow that begins well before a provider signs an employment agreement and continues uninterrupted throughout the provider’s time with the practice.
Pre-hire planning
Provider credentialing success is often determined before an offer letter is ever issued. At this stage, practices should:
- Define a realistic start date and anticipated payer mix to establish credible credentialing timelines.
- Identify which payers require full paneling—such as Medicare, Medicaid, and key local commercial plans—and which can be deferred or managed temporarily on an out-of-network basis.
- Decide who will own credentialing responsibilities, whether internal staff or an RCM partner like HealthCell, and confirm that the necessary bandwidth and tools are in place.
Early alignment here reduces downstream tension, particularly when providers expect to be fully operational on their first day in clinic.
Provider data collection
Once the agreement is signed, comprehensive data intake becomes the first operational priority. Typical documentation includes:
- Demographic details and government-issued identification
- Individual (Type 1) NPI, along with confirmation of the practice’s Type 2 NPI and tax ID
- Complete education and training history, including medical school, residencies, and fellowships
- Active state licenses and controlled substance registrations with expiration dates
- DEA registration and any state-specific prescribing identifiers
- Board certifications and examination dates
- Five to ten years of work history, with explanations for any gaps
- Malpractice insurance coverage and loss runs
- Hospital privileges, when applicable
- CVs, references, and disclosures of prior sanctions or disciplinary actions
Incomplete or inconsistent intake packets are among the most common causes of stalled or rejected credentialing submissions.
Primary source verification (PSV)
Primary source verification validates credentials directly with issuing organizations rather than relying on submitted documents alone. Depending on payer and accreditation standards, PSV typically includes:
- License and registration verification through state boards
- Confirmation of education and training with academic institutions and residency programs
- Verification of board certification status
- Review of federal and state sanctions databases
This step is a compliance cornerstone for many payers and accrediting bodies. Skipping it introduces unnecessary risk.
Internal review and approval
Practices that credential under their own medical staff bylaws—or operate under delegated credentialing arrangements—should maintain a structured internal review process. Common components include:
- Clearly defined criteria for initial appointment and reappointment
- Oversight by a credentialing committee or designated clinical leadership
- Documented evaluation of red flags, such as malpractice trends, employment gaps, or historical sanctions
Strong governance supports consistent decision-making and strengthens defensibility during audits or disputes.
Payer enrollment and effective dates
Once provider credentialing and internal approvals are complete, attention shifts to payer enrollment. This is where theory meets bureaucracy. Practices submit payer-specific applications or electronic transactions, each with its own idiosyncrasies. Even when CAQH supplies baseline data, payers still require unique forms, portals, and supporting documentation.
Medicare enrollment is processed through the PECOS system—or CMS-855 paper forms—using different applications for individual providers, group practices, and reassignment of benefits. Medicaid and commercial carriers add another layer, often requiring executed contracts, fee schedule acknowledgements, or explicit network participation decisions alongside credentialing materials.
Approval alone does not guarantee immediate reimbursement. Practices must verify effective dates and provider identifiers and ensure they align precisely with the first date of service they intend to bill. Miss that detail, and claims can stall before they ever reach adjudication.
Recredentialing and ongoing monitoring
Credentialing is continuous. It does not end with an approval letter.
Most payers mandate recredentialing every two to three years, a process that frequently mirrors the initial submission in both scope and scrutiny. CAQH compounds the cadence by requiring providers to re-attest to their profiles at least every 120 days—180 days in Illinois. Failure to do so can render a profile expired and effectively invisible to payers.
Licenses and certifications add further complexity. State licenses, DEA registrations, board certifications, and malpractice policies all carry expiration dates that must be monitored and renewed without lapse. Medicare and other payers also require prompt reporting of material changes, including address updates, ownership transitions, and adverse actions.
To manage this perpetual motion, many practices engage provider credentialing and RCM specialists like HealthCell. Centralizing these responsibilities reduces manual tracking, limits operational blind spots, and helps prevent the revenue loss and compliance findings that often trace back to credentialing oversights.
Medicare and PECOS: A Heightened Priority in 2026
For many practices, Medicare remains a financial cornerstone. At the same time, CMS has tightened oversight and sharpened enforcement. The result is a narrower margin for error, making Medicare enrollment a credentialing domain that warrants deliberate, ongoing attention.
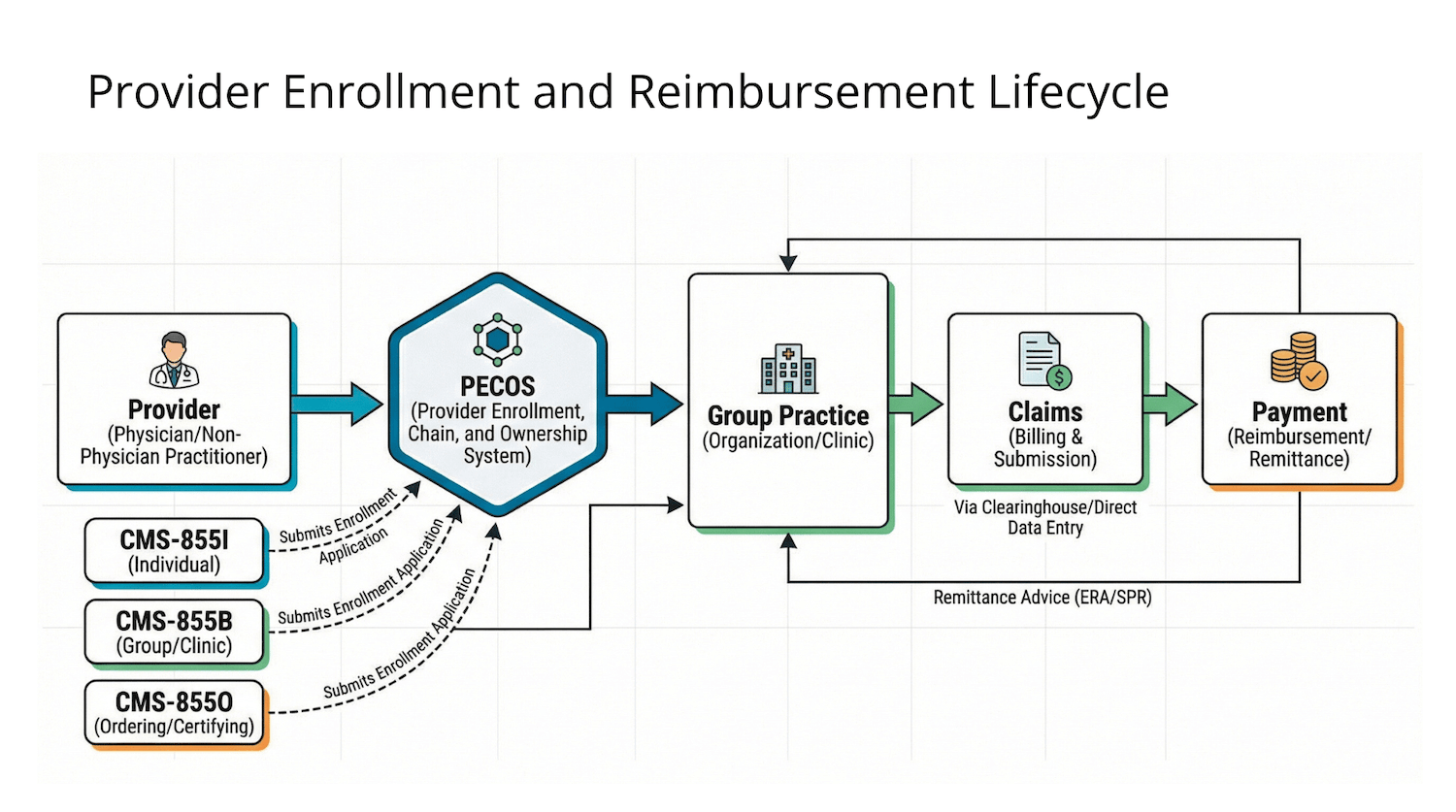
Understanding PECOS
The Provider Enrollment, Chain, and Ownership System (PECOS) is CMS’s centralized platform for Medicare enrollment and maintenance. Individual physicians and non-physician practitioners enroll through the CMS-855I application or its PECOS equivalent. Group practices enroll via CMS-855B. To allow the practice to receive payment, providers must formally reassign benefits from their individual enrollment to the group.
Absent an accurate and active PECOS record, Medicare claims will not adjudicate. There are no workarounds.
Application types and associated fees
Medicare enrollment relies on several distinct application types, including:
- CMS-855I for individual physicians and non-physician practitioners
- CMS-855B for group practices and other organizational suppliers
- CMS-855O for providers who order or certify services but do not submit claims directly
Certain institutional enrollments are subject to CMS application fees. These fees, along with acceptable payment methods, are updated annually and published by CMS.
Revalidation and change reporting
Medicare requires routine revalidation—typically every three to five years—during which providers must review, confirm, and update their enrollment data. In addition, practices are obligated to report material changes within prescribed timeframes, often within 30 days for significant events, including:
- Changes in ownership or controlling interest
- Opening or closing practice locations
- Adverse legal actions such as sanctions, revocations, or exclusions
Failure to maintain current PECOS information can lead to revocation of billing privileges and retroactive payment recoupment, a risk that smaller practices frequently underestimate.
Given the complexity and regulatory sensitivity, many practices rely on RCM partners like HealthCell to manage Medicare enrollment workflows. This includes PECOS submissions, revalidation tracking, and coordination with billing teams to ensure continuity of reimbursement.
CAQH Best Practices for Small and Mid-Sized Practices
Because commercial payers lean heavily on CAQH data, disciplined management of CAQH profiles can meaningfully compress credentialing timelines and reduce friction across the enrollment process.
Building a strong CAQH profile
A durable CAQH profile is built on consistency and completeness. Key steps when creating or updating a profile include:
- Completing all demographic, professional, and practice location fields with data that aligns precisely across NPPES, PECOS, and payer applications.
- Uploading all required documentation, including active licenses, DEA registration, malpractice certificates, and current CVs.
- Authorizing access for all relevant health plans so payers can retrieve information without initiating separate requests.
When CAQH data is accurate and comprehensive, credentialing turnaround times shorten and unnecessary payer correspondence declines.
Managing re-attestation and ongoing updates
CAQH requires providers to attest to the accuracy of their profile at least every 120 days—180 days for Illinois-based providers. Miss that deadline, and the profile is marked expired. An expired or un-attested profile can quietly create outsized problems, including:
- Removing the provider from payer credentialing queues
- Delaying recredentialing and network renewals
- Contributing to claim denials or payment holds when payers cannot validate provider data
To mitigate this risk, practices should maintain a shared calendar or dashboard that tracks CAQH attestation dates and material updates such as new locations, name changes, or license renewals. These checkpoints should be embedded into onboarding and offboarding workflows, not managed ad hoc.
HealthCell’s credentialing teams routinely integrate CAQH oversight into their standard operating procedures, helping providers remain continuously visible, accessible, and credential-ready across payer networks.
Delegated vs. Non-Delegated Credentialing
Whether a practice operates under delegated or non-delegated credentialing arrangements has a direct impact on accountability, workflow design, and overall timelines. The distinction matters more than many organizations realize.
Non-delegated (payer-managed) credentialing
In a non-delegated model, credentialing authority sits with the payer. Practices submit applications, maintain CAQH data, and respond to follow-up requests, but the payer controls primary source verification and committee review.
The upside is reduced internal infrastructure and lighter governance requirements. The tradeoff is diminished control. Timelines are often extended, bottlenecks are opaque, and practices have limited leverage to accelerate approvals when delays arise.
Delegated credentialing
Delegated credentialing shifts responsibility to the practice or its management entity under payer-defined standards. Instead of credentialing each provider directly, the payer audits the practice’s process and files for compliance.
Delegation can deliver tangible benefits. It often shortens the path to network participation by allowing practices to onboard providers according to internal timelines. It also promotes consistency across payer files, reducing duplicative effort.
That efficiency comes with a cost. Delegated arrangements demand formal policies, trained credentialing staff, reliable PSV workflows, and continuous audit readiness. For many small or independent practices, building that infrastructure in-house is impractical. As a result, organizations frequently rely on specialized RCM partners like HealthCell to provide CVO-style support and maintain audit-ready documentation while the practice retains oversight.
Common Provider Credentialing Pitfalls—and How to Avoid Them
Most credentialing disruptions are not novel. They are predictable, repeatable, and largely preventable. Independent practices tend to encounter the same pressure points again and again.
| Common Pitfall | Preventive Action |
|---|---|
| CAQH profile expired | Calendar-based re-attestation tracking |
| Provider scheduled too early | Enrollment-first go-live policy |
| Inconsistent data | Single source of truth |
| Medicare changes not reported | PECOS monitoring workflow |
Among the most frequent missteps:
- Incomplete submissions and inconsistent data across CAQH, NPPES, PECOS, and payer-specific forms, triggering rejections, clarification requests, and repeated resubmissions.
- Late starts, with providers scheduled to see fully insured patients before enrollment approval is secured.
- No centralized source of truth for credentialing data, resulting in version control issues, fragmented records, and missed recredentialing deadlines.
- Neglected CAQH re-attestation, allowing profiles to expire and providers to quietly disappear from payer queues.
- Underestimating Medicare complexity, particularly revalidation and change-reporting requirements that can lead to revocations or retroactive recoupments.
Practices that approach credentialing as a disciplined operational function—often with support from RCM partners like HealthCell—encounter fewer surprises when providers go live and far less disruption once billing begins.
Building a Practical Credentialing Playbook
Every practice should convert guidance into action. That means translating principles into a concrete, living playbook tailored to the practice’s specialty mix, geographic footprint, and payer landscape.
Roles and responsibilities
Credentialing functions best when ownership is explicit. At a minimum, practices should define:
- A credentialing lead, either in-house or a HealthCell credentialing specialist, accountable for timelines, CAQH management, payer correspondence, and internal status updates.
- A billing or RCM liaison responsible for ensuring enrollment effective dates flow accurately into practice management systems and claim edits.
- Clinical or medical staff leadership charged with credentialing review, approvals, and ongoing oversight.
Clear accountability reduces ambiguity and keeps critical tasks from slipping through operational gaps.
Tools and tracking
At baseline, practices should maintain a centralized credentialing tracker that captures, for each provider:
- Payers, application submission dates, approval dates, and effective dates
- CAQH ID numbers and most recent attestation dates
- License, DEA, board certification, and malpractice expiration dates
- Medicare and Medicaid enrollment identifiers and revalidation timelines
More mature organizations may leverage dedicated credentialing platforms or their RCM partner’s systems. Still, even a carefully maintained spreadsheet outperforms fragmented, ad hoc tracking—and often by a wide margin.
When to partner with a credentialing service
Very small practices may manage credentialing internally for a time. Eventually, scale and complexity intervene. Many organizations decide to partner with credentialing services once they begin to:
- Add new providers on a regular cadence
- Operate across multiple states or manage a dense, fragmented payer mix
- Experience revenue disruption or compliance exposure tied directly to credentialing delays
At that inflection point, external support becomes less a convenience and more a stabilizing force. HealthCell’s credentialing services often operate as a seamless extension of the practice, managing provider intake, CAQH administration, primary source verification coordination, payer enrollment, PECOS workflows, and ongoing monitoring. Policy direction and clinical oversight remain with the practice, while the operational burden is lifted.
Provider Credentialing FAQs
What is provider credentialing in healthcare?

Provider credentialing is the process of verifying a clinician’s education, training, licenses, certifications, work history, and professional standing to confirm they are qualified to deliver patient care and meet payer and regulatory requirements.
How is provider credentialing different from payer enrollment?
Credentialing verifies qualifications and compliance, while payer enrollment registers a provider with an insurance plan so claims can be reimbursed. A provider must be credentialed before enrollment can be completed.
How long does provider credentialing typically take?
Credentialing timelines vary by payer but commonly range from 60 to 180 days. Medicare and Medicaid enrollments often take longer, particularly if applications require corrections or additional documentation.
Can a practice bill for services before credentialing is complete?
In most cases, no. Services rendered before credentialing and enrollment effective dates are frequently denied, and many payers do not allow retroactive enrollment.
How often does recredentialing occur?
Most payers require recredentialing every two to three years. The process often mirrors initial credentialing and requires updated documentation and verification.
When should a practice consider outsourcing credentialing?
Practices often outsource credentialing when onboarding providers frequently, operating across multiple states, managing complex payer mixes, or experiencing revenue disruption due to credentialing delays. Specialized partners like HealthCell can manage credentialing workflows while reducing administrative burden.